|
A
Acanthosis
nigricans |
Acne vulgaris | Acrochordons
| Actinic cheilitis | Actinic
keratoses | Actinic lentigines
| Age Spots (go to actinic lentigines)
| Ageing skin | Albinism
| Allergy | Alopecia
| Alopecia areata | Anaphylaxis
| Androgenetic alopecia
| Angioedema | Angiokeratomas
| Angular cheilitis | Annular
erythema | Aphthous ulcers
| Aplasia cutis | Athlete's
foot (see tinea pedis) | Atopic
dermatitis | Atopic eczema (go to atopic
dermatitis) | Atrophie
blanche
ACANTHOSIS NIGRICANS
This is a skin condition
that causes a dark velvety thickening of the skin on the neck,
armpits and groin.
Causes
- Endocrine of hormonal
abnormality.
- Inherited disorder.
- Drug induced eg.,
from nicotinic acid, oral contraceptives and stilboestrol.
- Obesity when it is
called pseudoacanthosis nigricans.
- Underlying cancer.
Symptoms
- Thick, grey or black
velvety skin on the neck, groin or armpits.
- In acanthosis nigricans
due to underlying cancer, there may be velvety thickening inside
the mouth, as well.
 |
Acanthosis nigricans affecting
the armpit in a patient with underlying cancer.
Click
on image for larger view. |
What you can
do
- You chould consult
a doctor to determine the cause.
- Weight reduction may
improve pseudoacanthosis nigricans.
What the doctor
may do
- Determine the cause.
- Treat the underlying
cause.
TOP
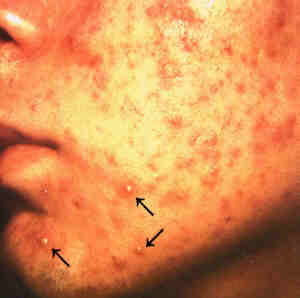
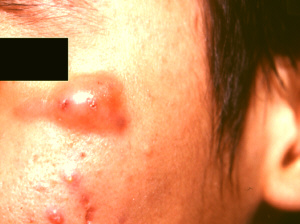
ACNE
VULGARIS
Acne vulgaris or acne
is the medical term for pimples. It usually begins in puberty
in both sexes when the adrenal glands (which sit on top of the
kidneys) and sex organs start producing androgens (male hormones).
Acne is most common between the ages of 16 - 18 and becomes less
common thereafter. However, about 1 in 5 adults, especially women
continue to be troubled by acne, although it is usually less
severe.
Acne usually affects the face and occasionally, the neck, chest,
shoulders and back, as well. Treatment is not a cure but it can
the problem and reduce the risk of permanent scars.
TOP
ACROCHORDONS
Acrochordon (papilloma)
is the medical term for a skin tag. This is a harmless skin growth,
commonly seen in middle-aged adults.
- Causes
- Uncertain but the
following factors appear to influence it's development:-
- Familial tendency.
- Obesity.
Symptoms
- Small fleshy skin-coloured
tags.
- Occur on areas subjected
to friction such as the neck, armpits, groins and under the breasts
and occasionally, on the eyelids as well.
- They may increase
in numbers during pregnancy.
 |
Acrochordons (skin tags)
on the neck.
Click
on image for larger view. |
Complications
- Torsion (twisting
on itself) causing inflammation and pain.
What you can do
- You can consult a
doctor for removal.
- Do nothing since skin
tags are cosmetic in nature.
What the doctor
may do
- Remove them using
surgical excision, electrosurgery,
carbon dioxide laser
or liquid nitrogen.
TOP
ACTINIC CHEILITIS
This is a form of actinic
keratosis affecting the lower lip. Like actinic
keratoses, it is also more common among fair-skinned individuals,
especially those of Celtic origin.
Cause
- Sun-damage.
Symptoms
- Redness, scaling,
cracking and crusting of the lower lip.
Complications
- May develop into a
squamous cell cancer.
What you can do
- You should consult
a doctor.
- Use sunscreen-containing
lip balms or lip sticks.
What the doctor
may do
- Perform a skin biopsy
to confirm the diagnosis.
- Counsel you about
sun protection.
- Excise (cut) or treat
with the carbon dioxide
laser or electrosurgery.
TOP
ACTINIC KERATOSES
Actinic keratoses or
solar keratoses are precancerous skin growths found on areas
most exposed to the sun such as the face, ears, sides of the
neck and back of the hands and forearms. The term actinic
cheilitis is used when it affects the lower lip. Actinic
keratoses are more common in the elderly because of years of
exposure to the sun and in fair-skinned individuals, especially
those of Celtic origin.
Cause
- Sun-damage.
-
- Symptoms
- Red or yellow-brown,
scaly patches which feel coarse like sandpaper.
- Other signs of chronic
sun damage such as solar elastosis, senile comedones
(whiteheads and blackheads) and telangiectasias may be present.
- Cutaneous horns are a variety of actinic keratoses.
They project out of the skin rather like a small horn.
-
 |
Actinic keratosis on the
scalp
Click
on image for larger view |
- Complications
- May develop into a
squamous cell cancer.
What you can do
- You should consult
a doctor.
- Protect your skin
against further sun-damage (see sun
protection).
What the doctor
may do
- Perform a skin biopsy
to confirm the diagnosis.
- Counsel about sun protection.
- Treat with topical
5-fluorouracil, liquid
nitrogen, electrosurgery
and curettage (scraping),
dermabrasion (skin
planing), laser resurfacing
or chemical peels.
- Examine the skin carefully
for skin cancers.
- TOP
ACTINIC LENTIGINES
Actinic lentigines,
senile lentigines, solar lentigines, "liver spots"
and "age spots" are different terms for the same condition.
They occur on the sun-exposed skin of the middle-aged and elderly.
Causes
- Sun-damage.
Symptoms
- Light or dark brown
blotches measuring 4 - 30 mm in size.
- Affects the sun-exposed
areas, especially the face, back of the hands, the forearms,
upper back and chest.
- Signs of chronic sun-damage
such as telangiectasias,
solar elastosis
and coarse wrinkles are often
present.
 |
Actinic lentigines.
Click
on image for larger view. |
What you can
do
- You can consult a
doctor for remioval.
- Protect your skin
against further sun-damage (see sun
protection ).
Caution
- Lentigo maligna appears as a slowly growing
flat dark patch with an irregular and indistinct border and various
shades of brown, tan and black. It occurs most commonly on the
face or neck of an elderly person and can develop into malignant
melanoma.
What the doctor
may do
- Perform a skin biopsy
if the diagnosis of lentigo is uncertain or if there is a possibility
of lentigo maligna.
- Counsel about sun protection.
- Remove or lighten
for cosmetic reasons using a number of different methods:
-
TOP
AGEING
SKIN
Skin ageing may be
divided into two types:
- Intrinsic ageing
which is genetically
determined and
- Photoageing (dermatoheliosis) which is caused by excessive
exposure to the sun. Fair-skin individuals and those occupationally
or recreational exposed to the sun are likely to develop photoageing
early. Eighty per cent of the signs of ageing is believed to
be caused by sun damage. Accordingly, the best way to delay ageing
is to minimise exposure to the sun (see sun
protection).
Symptoms
The symptoms depend on the site of damage:
-
- Epidermis (superficial
skin)
-
- Melanocytes (pigment
cells)
-
- Connective tissue
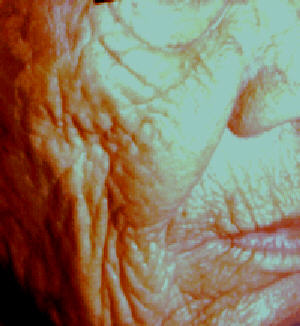 |
Coarse wrinkles due to
photoageing.
Click
on image for larger view. |
- Sebaceous glands
-
- Hair
-
- Blood vessels
-
- Subcutaneous fat
- Fat atrophy leading
to sunken cheeks, thinned skin.
What you can do
Obviously you cannot prevent ageing but the following measures
may help:
-
- Avoid sun-damage (see
sun protection).
- Get enough sleep and
rest.
- Exercise
- Healthy diet.
- Don't smoke.
- Don't take too much
alcohol.
- Don't do drugs.
TOP
ALBINISM
This is a rare inherited
condition caused by the partial or total lack of melanin. The
most common form of albinism is called oculocutaneous albinism.
Partial albinism is much rarer and affects only the skin, the
hair or the eyes. Ocular albinism affects the eyes alone.
Causes
- Inherited defect in
the synthesis of the skin pigment, melanin. Oculocutaneous albinism
and ocular albinism have different modes of inheritance - autosomal
dominant, autosomal recessive or X-linked.
Symptoms
- In severely affected
cases, the skin and hair are snowy white.
- The iris (the area
of the eyes surrounding the pupil) and the retina (back of the
eyes) are white and the eyes cannot tolerate bright lights and
are affected by nystagmus (abnormal jerky eye movements), squint
and myopia (short-sightedness).
- Ocular albinism affects
the eyes alone.
Complications
- There is a high risk
of skin cancer developing in oculocutaneous albinism because
the skin lacks the melanin that shields off harmful ultraviolet
rays.
What you can do
- You should consult
a doctor.
- Protection against
the sun is very important because of the risk of skin cancer
developing (see sun protection).
What the doctor
may do
- Provide genetic counseling
and advice on sun-protection.
- Follow-up closely
for the developing of skin cancers.
TOP
ALLERGY
Allergy is an abnormal
reaction to substances that are normally harmless or beneficial
to the body.
- Cause
- Normally, our bodies
produce antibodies in response to attack by a potentially harmful
foreign substance such as viruses and bacteria. In the case of
an allergy, however, antibodies are produced against substances
that are harmless or good for the body (for example, food items
or a particular treatment). These antibodies combine with the
substance (known medically as the allergen) and this sets
off a chain of chemical reactions that lead to the release of
histamine, the chemical that produces most of the symptoms of
an allergy. The allergen may be a substance taken into the body
such as a drug or food item, dust, venom from an insect bite
(see bites and
stings) or a substance that has been in contact with the
skin such as costume jewelry, cosmetics or plants (see contact
dermatitis). Theoretically, any substance can cause an allergy,
including one the person has taken or been in contact with before
without problems.
Symptoms
- Contact
dermatitis
- Eczema or itchy red scaly or weepy patches.
- Urticaria (weals or nettle rash).
- Morbilliform (measles
like) rash.
- Purpura.
- Vasculitis.
- Erythema
multiforme.
- Erythema
nodosum.
- Fixed
drug eruption.
Complications
- Anaphylaxis - A severe reaction resulting
in shock, suffocation and even death.
What you can do
- You should consult
a doctor.
- Take antihistamine
to relieve itch.
- Apply calamine lotion.
- Go to the nearest
Accident and Emergency Department if you have generalised urticaria
or swelling of the eyelids, lips or difficulty breathing or if
there are signs of anaphylaxis developing.
What the doctor
may do
- Hospitalise severe
cases of allergy.
- Give antihistamine
injections.
- Prescribe systemic
steroids.
- Determine the cause
of the allergy with the aid of patch
tests, skin tests
(prick or intradermal tests) or RAST
tests if necessary.
- Desensitise selected
cases. This is done by injecting small doses of an allergen in
order to train the body to accept it. However, desensitisation
is only available for some allergens such as house dust, poison
ivy and bee
and wasp stings and there is a small risk of desensitisation
causing a severe reaction.
Prevention
- Avoid the substances
you are allergic to.
- Apply for a medical
alert (for example, Medik Awas) card and carry it on your person
all the time. Get the application form from your doctor.
- Inform your doctor,
dentist, and pharmacist each time you see them.
- Inform your relatives
about your allergy, as well.
TOP
ALOPECIA
Alopecia is the medical
term for hairloss. Doctors divide alopecia into non-scarring
and scarring alopecia. Scarring alopecia is due to inflammation
causing scarring and destruction of the hair follicles. The causes
include:
- TOP
ALOPECIA
AREATA
Alopecia areata causes
hairloss in round patches. It usually affects young adults and
children and may be associated with a family history of alopecia
areata or other autoimmune disorders (self-allergies) such as
vitiligo and thyroid disease (Hashimoto's thyroiditis).
Cause
- Alopecia areata is
believed to be an autoimmune disorder in which the body produces
antibodies that attack the hair follicles as though they were
foreign.
Symptoms
- Solitary or multiple
well-defined circular bald patches on a normal or occasionally,
slightly reddish skin.
- Broken hairs may be
seen in the bald patch. They have broken-off stubbled ends and
are often referred to as exclamation mark hairs because of their
appearance.
- The scalp is most
commonly affected. Less commonly affected areas include the eyebrows,
eyelashes, pubic hair and beard.
- Complications
Alopecia areata may occasionally lead to widespread hairloss
causing:
- Alopecia totalis which causes total baldness
of the scalp.
- Alopecia universalis where the hairloss affects
the entire body including eyebrows, armpit and the pubic hair.
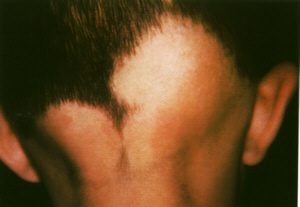 |
Muliple patches of alopecia
areata.
Click
on image for larger view. |
Severe alopecia areata
progressing to alopecia universalis.
Click
on image for larger view. |
| |