|
C
Cafe
au lait patches
| Candidiasis | Canities
| Canker sores (go to aphthous
ulcers) | Capillaritis (go to pigmented
purpuric dermatosis) | Cat scratch
fever | Cavernous haemangioma
| Celluilte | Cellulitis
and erysipelas | Chalazion | Chapped
skin (go to xerosis) | Chemical
peels (go to treatments, chemical
peels) | Cherry angioma |
Chickenpox (go to varicella)
| Chilblains | Chloasma (go to melasma) | Cold sores (go to herpes
simplex virus infection) | Comedones
| Congenital naevi | Connective
tissue naevi | Contact dermatitis
| Corns and callosities
| Cradle cap | Cutaneous larva migrans
(go to larva migrans) | Cuts and grazes | Cysts
CAFE AU LAIT PATCHES
Cafe au lait, as the
name suggests refers to white coffee-coloured patches.
Cause
- Unknown
- May be a sign of neurofibromatosis, an inherited
disease affecting the nerve fibre sheaths.
Symptoms
- Light coffee-coloured
patches hence, the name cafe au lait which is French for white
coffee.
- Six or more cafe au
lait patches that are larger than 1.5cm in diameter may indicate
neurofibromatosis (von Recklinghausen's disease). Other
signs of neurofibromatosis
include multiple soft swellings called neurofibromas anywhere
on the body and sometimes in the central nervous system where
it can cause visual problems, hearing problems and epilepsy (fits)
and spinal deformities.
 |
Cafe au lait patches
Click
on image for larger view. |
What you can
do
- You should consult
a doctor, especially if there is a family history or there are
signs of neurofibromatosis.
- Seek treatment from
the doctor if the patches are cosmetically disturbing.
What the doctor
may do
- Exclude neurofibromatosis.
- Use one of the pigment lasers to remove
the patch.
TOP
CANDIDIASIS
Candidiasis, also known
as moniliasis or thrush is an infection caused by a yeastlike
fungus called Candida albicans.
- Causes
- Candida albicans is a yeast that is often found
in the normal vagina, mouth and intestines. It does not usually
cause any symptoms until certain conditions favour its proliferation
(see predisposing factors).
-
- Predisposing factors
- Frequent contact with
water (see paronychia).
- Anaemia.
- Diabetes.
- Tight foreskins that
are difficult to retract (pull back) to clean.
- Warm moist macerated
body fold areas, especially in overweight persons.
- Napkin
dermatitis.
- Hormonal change, for
example, during pregnancy and while taking the birth control
pill.
- Oral antibiotics which
kill off the harmless bacteria that normally keeps Candida
albicans in check.
- Elderly persons wearing
poorly fitting dentures.
- Lowered resistance
caused by anticancer drugs and immunosuppressive
drugs including systemic steroids
and AIDS (acquired immune deficiency syndrome).
- Symptoms
The symptoms of candidiasis vary according to the sites affected:
- Skin folds (candidal
intertrigo)
- Well defined moist
red patches in body fold areas such as the groins, buttocks,
under the breasts, between the toes and in the armpits.
- Small red papules
(pimply bumps) or pustules (pusheads) may be seen outside the
main area. These are called satellite papules.
- Itching.
-
- Mouth
(oral candidiasis)
- Red moist patches
patches covered by a white cheesy membrane (which can be scraped
off, leaving a bleeding inflamed surface) inside the cheeks or
on the tongue.
- Pain and a burning
sensation.
-
- Lips
-
- Penis (candidal
balanitis)
- Red spots and white
patches on the head of the penis and under the foreskin.
- Discharge.
- Itching.
-
- Vulva and vagina
(vulvovaginal candidiasis)
- Thick white or yellow
vaginal discharge.
- Itchy, sore, red,
swelling of the labia (vaginal lips).
- Soreness during intercourse.
-
- Nail folds (candidal
paronychia)
- Redness, swelling
and tenderness of the nailfolds (see paronychia).
What you can do
- You should consult
a doctor.
- Loose weight if obese.
- Keep diabetes under
control. Follow the diet regimen recommended by the doctor or
dietitian and take the medications/injections regularly.
- If possible, try to
correct the predisposing factors.
What the doctor
may do
- Confirm the diagnosis
by examining skin scrapings under the microscope or by culture.
- Rule out underlying
medical problem.
- Circumcise patients
with recurrent balanitis who have tight foreskins.
TOP
CANITIES
This is the medical
term for greying of the hair.
Causes
- Natural ageing process.
- Premature ageing which
is defined as ageing in the early 20s may be due to genetic factors
or pernicious anaemia, a disease caused by the lack of intrinsic
factor which is needed for the absorption of vitamin B12.
- Vitiligo may also affect the melanocytes
in the base of the hair follicles and cause the hairs in that
patch to become white.
What you can do
- Nothing, live with
it.
- See a hairdresser
to get the hair dyed.
- Consult a doctor if
greying is premature.
What the doctor
may do
- Rule out underlying
causes in cases of premature greying.
TOP
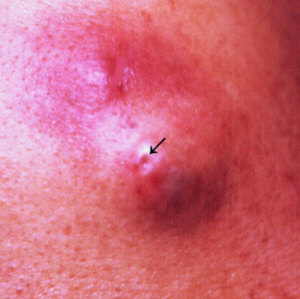
CAT SCRATCH FEVER
This is an illness
that occurs after a scratch or bite from a cat.
Cause
- Bacterial infection
transmitted by a cat bite or scratch. The cat itself is usually
healthy. The infection is usually temporary.
Symptoms
- Small red papule or
blister at the site of injury.
- Swollen painful lymph
glands near the site about 3 - 10 days after the bite or scratch.
- May be fever, rash,
and headache.
What you can do
- You should consult
a doctor.
What the doctor
may do
- Take a biopsy of the
enlarged lymph gland.
- Perform a skin test
with the cat-scratch antigen.
TOP
CAVERNOUS HAEMANGIOMA
The cavernous haemangioma
is a deep haemangioma (vascular birthmark) that usually affects
young children. It usually appears at birth and may occur anywhere
on the body, especially on the head and neck.
Cause
- A type of vascular
birthmark. Abnormally large and malformed blood vessels develop
in the deep dermis and subcutaneous tissue.
Symptoms
- Deep blue to purple
(sometimes skin coloured) soft compressible growth.
- Unlike strawberry
marks, cavernous haemangiomas do not usually disappear completely
with age.
 |
Cavernous haemangioma.
Click
on image for larger view |
Complications
- Cosmetically disfiguring,
especially when it occurs on the face.
- May obstruct vision
if it occurs around the eyes.
- Ulceration and bleeding
may follow trauma.
- Underlying tissue
may overgrow resulting in enlargement of the affected limb. This
is known as Klippel-Trenaunay-Weber syndrome.
- Sometimes platelets
(special white blood cells that help clotting) get caught and
destroyed in the haemangioma resulting in thrombocytopaenia purpura.
This is known as Kasabach-Merritt syndrome).
What you can do
- You should consult
a doctor.
What the doctor
may do
- Prescribe systemic
or inject intralesional
steroids to shrink the haemangioma.
- Destroy the abnormal
blood vessels using electrosurgery
or vascular lasers.
TOP
CELLULITE
Cellulite refers to
the uneven dimpled skin that results from lumpy deposits of fat
in the skin. It usually occurs on the hips, buttocks and thighs
of women.
Cause
- Cellulite is common
in women because their fat is separated into vertical compartments
by fibrous bands running from the skin to the muscle fascia (layer)
beneath. It is believed that poor blood circulation causes these
fat compartments to swell while the fibrous bands pull the skin
down. This causes the skin to develop mattress-like protrusions
and dimples, respectively.
Symptoms
- Lumpy fat deposits
in areas such as the buttocks, hips and thighs.
- The skin usually shows
a dimpled, orange-peel appearance.
What you can do
- Nothing, live with
it.
- Cellulite become more
obvious with obesity. Regular exercise and weight reduction is
helpful.
- If the above doesn't
work which is not uncommon, consider seeing a doctor for liposuction
(fat suction).
What the doctor
may do
- Refer to a dietitian.
- Perform liposuction.
However, it must be emphasized that recurrence is very common
unless you exercise regularly and avoid putting on weight.
TOP
CELLULITIS AND ERYSIPELAS
Cellulitis and erysipelas
(St Anthony's fire) are acute bacterial infections of the skin.
Causes
- Cellulitis is usually
caused by the streptococcal bacteria, staphylococcal
bacteria or both.
- Erysipelas is caused
by streptococcal bacteria.
- The bacteria usually
enter through a small break in the skin.
-
- Predisposing factors
- Diabetes.
- Intravenous drug abuse.
- Poor immunity.
-
- Symptoms
- Cellulitis:
- Red, hot, swollen,
tender area sometimes associated with lymphangitis (red lines
spreading upwards).
- The margins are not
well-defined.
- Fever and chills.
- Enlarged tender lymph
glands draining the region.
-
- Erysipelas:
- Red, hot, swollen,
tender patch with a raised sharply defined edge.
- Fever may be high
and associated with chills.
- There may be malaise
(feeling of illness), headache and vomiting.
- Enlarged tender lymph
glands draining the region.
Complications
- Certain strains of
the streptococcal bacteria can cause glomerulonephritis (kidney
inflammation).
Key point
- Rapidly progressive
cases with necrosis (dead skin) need to be differentiated from
ecthyma gangrenosum (caused by the pseudomonas
bacteria) and necrotising fasciitis caused by a particularly
virulent form of the streptococcal bacteria dubbed the "flesh-eating
bacteria").
What you can do
- You should consult
a doctor.
- Apply a warm compress
to the area two or three times a day.
What the doctor
may do
- Take a culture to
choose the best antibiotic to use.
- Treat with antibiotics.
- Hospitalise severe
cases for management.
TOP
CHALAZION
This is a relatively
cyst affecting the eyelid.
Cause
- Obstruction of one
of the meibomian glands in the eyelids.
Symptom
- Round cyst on the
eyelid.
- If infected, the swelling
becomes painful and red.
What you can do
- You should consult
a doctor.
- Apply warm compress
for 20 minutes if the swelling is inflamed.
What the doctor
may do
- Prescribe antibiotic
drops/ointment.
- Cut and drain large
chalazions.
TOP
CHERRY
ANGIOMAS
Cherry angiomas, senile
angiomas or Campbell de Morgan spots are bright red dome-shaped
bumps on the trunk and upper parts of the limbs. They usually
appear during middle age and increase in number with age.
Cause
- Enlarged small capillaries
in the skin due to ageing.
Symptoms
- Bright red dome-shaped
bumps.
 |
Cherry angiomas.
Click on image for larger view |
Complications
- Minor - may bleed
a little if traumatised.
What you can do
- You can consult a
dotor.
- Avoid scratching them.
- Decide not to have
any treatment as cherry angiomas are cosmetic.
What the doctor
may do
- Destroy with electrosurgery,
the carbon dioxide laser
or one of vascular lasers.
TOP
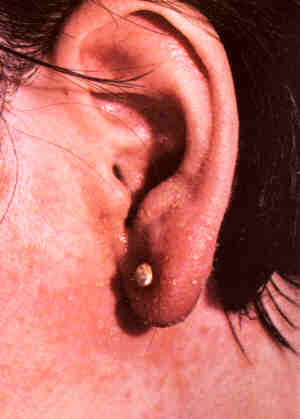
CHILBLAINS
Chilblains (also called
perniosis) is an abnormal response to moderately cold temperatures.
It is more common in temperate climates and usually affects the
extremities, including the earlobes and nose. Children, especially
young girls are more likely to be affected. Chilblains is self-limiting
and usually resolves within 1 or 2 weeks.
Cause
- The body normally
reacts to cold by cutting down the blood flow to the skin. In
chilblains, this reaction is exaggerated such that certain parts
of the skin are so deprived of blood that they become red and
swollen.
Predisposing factors
- Family tendency.
- Poor circulation due
to diabetes, smoking or atherosclerosis..
- Poor nutrition.
- Collagen vascular
diseases such as systemic lupus
erythematosus
Symptoms
- Itchy, red or purple
swellings. In severe cases, there may be blistering and ulceration.
- Usually affects the
legs and ends of the body such as the digits, heels, nose and
ears.
- Itching, burning or
pain.
What you can do
- You should consult
a doctor.
- Prevention is very
important as treatment is not very effective once chilblains
has developed.
Prevention
- Avoid cold environments.
Move to a warm climate.
- Keep the whole body,
especially the fingers and toes warm by wearing gloves and stockings.
Avoid wearing open-ended sandals when the weather is cold.
- Avoid wearing tight-fitting
shoes.
- Exercise regularly.
- Stop smoking.
What the doctor
may do
- Exclude underlying
circulatory disorder and diabetes.
- Prescribe topical
steroids.
- Prescribe oral nifedipine
to dilate the constricted blood vessels.
TOP
COMEDONES
Comedones are the blackheads
and whiteheads that occur in acne vulgaris (pimples). They usually
occur on the face, chest and back. Senile comedones are those
that occur on the sun-damaged skin of the elderly.
Causes
- Acne
vulgaris.
- Sun-damage (solar
or senile comedones).
Symptoms
- Open comedones - whiteheads.
- Closed comedones -
blackheads.
- Solar or senile comedones
usually occur on leathery, yellow sun-damaged skin of elderly
individuals. This condition is called Favre Racouchot syndrome.
 |
Closed comedones (whiteheads)
due to acne vulgaris.
Click
on image for larger view |
Complications
- Acne associated comedones
may rupture and develop inflamed papules (inflamed pimply bumps),
pustules (pusheads), nodules and cysts.
What you can do
- Apply topical anti-acne
products containing benzoyl peroxide, sulphur or salicylic acid
which help to peel the skin.
- Do not squeeze comedones
as this may cause them to rupture, increasing the risk of inflammation
and scarring.
- Avoid using moisturisers
routinely. If you must, use only water-based moisturisers.
- Consult a doctor if
there is no improvement.
- Protect the skin against
the sun to reduce the risk of senile comedones developing.
What the doctor
may do
- Prescribe topical
tretinoin (vitamin A
acid).
- Use a comedo extractor
to extract comedones under sterile conditions.
- Perform superficial
chemical peels.
TOP
CONGENITAL NAEVI
Congenital naevi (plural
for naevus) or congenital moles are pigmented birthmarks that
appear at or within a year of birth. They vary in size but are
generally larger than ordinary moles.
Congenital naevi may occur anywhere on the body and may have
a hairy surface.
TOP
CONNECTIVE TISSUE NAEVI
These are rare developmental
abnormalities involving the connective tissues.
- Cause
- Developmental abnormality
involving the connective tissue.
Symptoms
- Elastoma - a plaque (raised patch)
comprised of smooth skin-coloured papules (pimply bumps). Usually
occurs on the trunk.
- Collagenoma - yellowish raised patch on
the upper trunk or limbs. Usually appears at or soon after birth.
- Shagreen patch - a yellowish thickening of
the skin. Usually occurs on the lower back. May be associated
with tuberous sclerosis, an autosomally inherited disorder causing
an acne like eruption on the face (adenoma sebaceum), epilepsy,
mental retardation (in some patients) and subungual fibromas
(overgrowths of fibrous tissue on the sides of the nails).
- Buschke-Ollendorf
syndrome -
multiple yellow-orange papules (pimply bumps), nodules or plaques
(raised patch) on the thighs, buttocks and abdomen. Occurs in
early adult life. Inherited by autosomal dominant transmission
which means only one parent need to be affected and the offsprings
have a 1 in 2 chance of inheriting and developing the disorder.
What you can do
- You should consult
a doctor.
What the doctor
may do
- Perform a skin biopsy
to confirm the diagnosis.
- No treatment is needed.
- Excise or treat with
the carbon dioxide laser
or electrosurgery.
TOP
CONTACT DERMATITIS
Contact dermatitis
is an eczema or dermatitis caused by contact with a substance.
It appears at the site of contact initially but may later spread
to other parts of the body.
Causes
- Allergic contact
dermatitis
where the dermatitis is caused by an reaction between the body's
immune system and the allergy causing substance (known as the
allergen). It takes 1 week to years for the body's immune system
to react and during this time (known as sensitisation), the skin
can appear completely normal. It is only on re-exposure that
the dermatitis develops. This is why a person may become allergic
to a substance he has used for years without problems. Common
causes of allergic contact dermatitis include:
-
- Metals
- Nickel - Allergy to
nickel is more common in women. Common sources of nickel include
costume jewelry, zips, jeans studs, metal spectacle frames, and
metal fasteners on brassieres, watch straps, belts. 12 carat
gold and silver are generally safe but 9 carat gold or white
gold contain nickel. Nickel allergy affects 5% of women.
-
- Chromates - A common
cause of contact dermatitis in men. It is found in cement, tanned
leather, photographic dyes, primer paint and anti-corrosives.
-
- Rubber additives -
Found in tyres, footwear, belts, condoms and gloves.
- Mercaptobenzothiazole
- Thiuram
- Paratertiarybutylphenol
-
- Resins, plastics and
adhesives
- Colophony - Plasters,
adhesive tapes, glue, varnish and polish.
- Epoxy resins - Usually
causes occupational
dermatitis.
- Formalin resins -
Used for water-proofing fabrics.
-
- Cosmetics
- Fragrance - These
include cinnamic alcohol, cinnamic aldehyde, musk ambrette, isoeugenol,
geraniol, oil of Bergamot, and many more. Fragrances are found
in many products including soap, deodorants, cosmetics, creams
and perfumes.
- Lanolin (wool fat)
- A type of fat derived from sheep oil glands. It is often used
in cosmetics and creams.
- Preservatives - These
include chemicals such as parabens, quarternium 15, diazolidinyl
urea and imidazolidynyl urea that are added to prevent the product
from going bad. They are often used in cosmetics, creams and
shampoos.
- Toluenesulfonamide
formaldehyde resin - Found in nail polish and causes rashes when
it comes into contact with the eyelids and neck before it has
dried.
-
- Dyes in clothings.
- Paraphenylenediamine
(PPD) - Blue, black dyes. PPD is alos used in black hair dye.
- Paratoluenediamine
- Red dyes.
- Azo dyes - Orange,
yellow and red dyes.
-
- Medicaments
- Neomycin - Found in
some antibiotic medication.
- Acriflavine - Used
in antiseptic lotions.
- 'Caine' local anaesthetics
- Used in some anti-itch products and haemorrhoids medication.
- Diphenhydramine -
Used in anti-itch products.
-
- Plants or of plant
source
- Chrsanthemums - May
cause a photoallergic contact dermatitis.
- Poison Ivy , cashews,
pistachios, mangoes.
- Chinese and Japanese
lacquer; oak, rosewood, primula.
- Tulip bulbs, garlic.
-
- Industrial chemicals
- A multitude of industrials, too many to be listed, may cause
contact dermatitis (see occupational
dermatitis).
-
- Irritant contact
dermatitis which
is due to the direct effects of the substance on the skin without
involving the immune system. Strong irritants such as acids and
alkalis can cause dermatitis after a short exposure whereas weak
irritants such as water, detergents, solvents, abrasive dusts
and coolants do so after repeated exposure over a longer period.
The latter variety is known as cumulative insult dermatitis.
Examples of cummulative insult dermatitis include "housewife's
dermatitis" and "bartender's hands".
- Photocontact dermatitis which is contact dermatitis
that occurs only in the presence of light. There are two types:
-
- Photoallergic
contact dermatitis
is a type of allergic contact dermatitis that takes place only
in the presence of light. The causes include musk ambrette in
male aftershave lotions and sunscreen chemicals such as PABA
or its esters and topical sulphonamides.
-
- Phototoxic
contact dermatitis
which occurs in the presence of light but does not involve an
allergic reaction. may be caused by certain perfumes, tar products,
plant psoralens (psoralens are light sensitising chemicals).
-
- Symptoms
- Contact dermatitis
begins at the site of contact but may spread to distant sites
if there is continued contact.
-
- Acute eczema - blisters, swelling and weeping.
- Chronic eczema - dry, red, scaly thickened
areas.
- Itching.
 |
Allergic contact dermatitis.
Click
on image for larger view |
Complications
- Secondary bacterial
infection.
What you can do
- You should consult
a doctor.
- Avoid scratching.
- Take antihistamines.
What the doctor
may do
- Determine the cause
using the history, appearance and with the aid of allergy tests
(patch tests).
- Prescribe topical
and in severe cases, even systemic steroids.
- Prescribe antibiotics
if there is a bacterial infection.
- If you are allergic
to nickel, the doctor may give you a nickel testing (dimethylglyoxamine)
solution for detecting the persence of nickel in metal objects.
Dampen a tissue with the solution and rub the object with it.
A pink colour on the tissue indicates the presence of nickel.
TOP
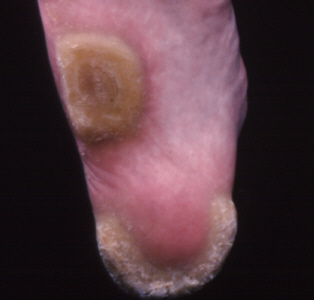
CORNS AND CALLOSITIES
Corns and callosities
are common thickenings of the skin seen most commonly on the
feet. Callosities may also develop on the hands of people who
constantly handle heavy tools.
Causes
- Repeated friction
and/or pressure causes the skin to thicken and harden.
Symptoms
- Calluses
- Thickening of the
skin.
- Cracking of the skin
and sometimes pain.
-
- Corns
- Thickened skin with
a central whitish core.
- Pain due to the hard,
central core pressing on the nerve endings in the feet when walking.
- Soft corns - a soft
whittish variety of corn occuring between the toes.
What you can do
- Eliminate friction
and pressure.
- Use products containing
salicylic acid (corn pads, paints and lotions) to soften the
thickened skin. Do not use these if you have diabetes or circulatory
problems.
- Regularly rub away
the thickened skin with a pumice stone or file. (See a doctor
if you have diabetes or circulatory problems because of the risk
of delayed healing and infection should you accidentally injure
the skin).
- Use protective felt
pads to relieve the pressure on the thickened skin and reduce
pain.
- Use small gauze pads
to separate the toes in the case of soft corns.
Prevention
- Wear protective gloves
when handling heavy tools.
- Take a rest between
heavy jobs.
- Wear proper fitting
shoes that are sufficiently wide at the front.
- Avoid high heels as
they increase the pressure on the forefeet and toes during walking.
What the doctor
may do
- Exclude warts.
- Relieve pain by removing
the thickened skin of a callus or the core of a corn.
- Inject intralesional
steroids into the centre of a corn.
- Inject implant
material such as collagen or silicone under the corn or callus
to act as a cushion.
- Correct arthritic
joints/deviated toes or surgically remove bony prominences that
are pressing on the thickened skin.
TOP
CRADLE
CAP
This is a common self-limiting
condition causing greasy crusts on the scalps of babies.
Cause
- It is a form of seborrhoeic dermatitis
in infants. Inadequate cleansing out of fear of injuring the
soft spot is contributory cause as it leads to an accumulation
of grease and scales.
Symptoms
- Thick, yellow, greasy
scales over the scalp, especially on the soft spot.
- There may be evidence
of seborrhoeic dermatitison
the face, neck, behind the ears and the napkin area.
- What you can do
- Soften the scales
with baby oil/olive oil overnight and brush the scales off with
a soft toothbrush.
- Keep the area clean
by shampooing regularly.
- Consult a doctor if
the condition gets worse.
What the doctor
may do
- Prescribe a mild topical
steroid.
TOP
CUTS
AND GRAZES
The skin has a unique
ability to prevent infection after minor injuries. Bleeding occurs
which help to wash away germs, then blood clots form a hard scab,
under which new skin grows to eventually close the wound.
Cause
- Cuts are caused by
sharp objects.
- Grazes are caused
by rough surfaces rubbing against the skin.
Symptoms
- Slight bleeding.
- Pain.
Complications
- Secondary bacterial
infection.
- Severe bleeding if
the larger blood vessels are cut.
- Scars and keloids.
What you can do
- Rinse under running
water or clean with a liquid antiseptic.
- Apply an antiseptic
cream.
- Stop bleeding by pressing
with a cotton pad for about 5 minutes.
- Consulat a doctor
if bleeding continues, if there is a large gaping wound that
needs stitching or if there is an infection.
What the doctor
may do
- Stop the bleeding.
- Stitch open wounds.
- Prescribe antibiotics
for infection.
- Give antitetanus toxoid
injections.
TOP
CYSTS
A cyst is a sac containing
fluid or semi-solid material. The common cysts of the skin are:
- Milia
- Sebaceous cysts (also called epidermal or
epidermoid cysts and wens).
- Pilar cysts.
Cause
- Damage or blockage
of the hair follicle.
- inheritance may play
a role in pilar cysts as they tend to run in families.
Symptoms
- Milia
- Pin-head size white
cysts resembling whiteheads.
- They occur most frequently
on the eyelids, cheeks and forehead of infants and middle-aged
women and at sites of trauma.
-
- Sebaceous cysts
- Skin coloured swellings,
sometimes with an opening through which a smelly creamy paste
may be expressed.
- They occur most commonly
on the face, ear, scalp, neck, back, upper trunk and scrotum.
-
- Pilar cysts
- Similar to sebaceous
cysts except more commonly found on the scalp and may run in
families. If pierced, a gelatin-like secretion which is non-smelly
may be expressed.
Complication
- Cysts may become infected
and painful.
What you can do
- Milia in children
can be left to resolve spontaneously.
- Consult a doctor if
you wish milia or cysts removed
What the doctor may do
- Extract milia by nicking
the surface with a scalpel blade and extracting the contents
with a comedo (blackhead) extractor.
- Destroy milia with
electrosurgery.
- Excise sebaceous cysts
and pilar cysts. The sac or cyst wall must be removed or the
cyst may recur.
- Treat infected sebaceous
cysts with antibiotics together with drainage, if necessary.
TOP |