|
T
Tattoo
removal | Telangiectasias | Telogen
effluvium | Tinea | Tinea
amiantacea | Tinea versicolor (go to pityriasis
versicolor) | Traction alopecia (go to traumatic
alopecia) | Traumatic alopecia
| Trichoepithelioma | Trichostasis
spinulosa
TATTOO
REMOVAL
Tattooing is sometimes
used to camouflage an underlying birthmark or blemish. More often
however, tattooing is done for decorative reasons and for creating
a permanent eyeliner or to alter the shape of the eyebrows and
even the lips. No problems arise until the owner wishes to have
a tattoo removed because he no longer wants it, because the shape
is wrong or because of an allergic reaction to the tattoo pigment.
Until the advent of pigment lasers, removal of tattoos was almost
impossible without the risk of scarring.
What you can do
- Think carefully before
tattooing because removal is difficult and costly.
- See a doctor if you
would like a tattoo removed.
What the doctor
may do
- Excise small tattoos.
- Use dermabrasion
(skin planing).
- Use salabrasian which
involves using salt to sand the skin rather like dermabrasion.
- Use pigment
lasers to destroy tattoo pigment without harming the neighbouring
tissues too severely and causing unacceptable scarring. This
is currently the best method of tattoo removal but is expensive
because of the high costs of laser machines.
TOP
TELANGIECTASIAS
Telangiectasias are
broken capillaries (tiny blood vessels) in the skin.
Causes
- Sun damage.
- Acne
rosacea.
- Connective tissue
diseases such as scleroderma.
- Overuse of strong
topical steroids.
- Radiation damage.
- Liver disease.
- Pregnancy and birth
control pills.
- Inheritance as in
Osler Weber Rendu disease.
- Prolonged standing.
Symptoms
- Spider telangiectasias
(spider naevi)
- Red dots with dilated vessels radiating outwards like the legs
of a spider. Compression of the central "body" results
in the telangiectasia disappearing. Usually occur on the face,
neck, and upper body.
- Common telangiectasias
- red wavy
lines of blood vessels on the nose and cheeks of fair-skinned
individuals and on the legs of women.
- Osler Weber Rendu
disease or
hereditary haemorrhagic telangiectasia is characterised by telangiectasias
around the lips, mouth, face, fingers, toes and nail beds and
in the mucous membranes of the nose and gastrointestinal tract.
It is inherited in an autosomal dominant fashion which means
that each child has a 50% chance of inheriting and developing
the disorder if one parent is affected.
 |
Spider telangiectasias.
Click
on image for larger view |
Complications
- Haemorrhage and anaemia
may occur in Osler Weber Rendu disease.
What you can do
- You should consult
a doctor to determine the cause.
- Use cosmetic to camouflage
facial telangiectasias.
- See a doctor if there
are signs of Osler Weber Rendu disease or for treatment of the
telangiectasias.
What the doctor
may do
- Exclude underlying
diseases.
- Treat with electrosurgery
or vascular lasers.
TOP
TELOGEN EFFLUVIUM
Telogen effluvium is
a diffuse, temporary type of hairloss which occurs 2 - 4 months
after the cause and resolves within 6 months of the cause being
eliminated.
Causes
Normally, hairs grow in 3 stages - anagen (growth stage), catagen
(transitional stage) and telogen (resting stage). Generally,
about 85% of the hairs are in anagen and 15% are in telogen (very
few are in catagen). Telogen effluvium occurs when many hairs
(as much as 70%) are pushed into one cycle so that they are eventually
all shed together. Such an alteration of the hair cycle may be
precipitated by:-
- Childbirth and cessation
of oral contraceptives.
- High fever.
- Major surgery.
- Underactive or overactive
thyroid gland.
- Haemorrhage (blood
loss).
- Iron deficiency anaemia.
- Crash dieting.
- Malnutrition.
- Chronic illness.
- Jet lag.
- Accident.
- Unusual stress.
- Drugs such as anticoagulants
(blood thinning drugs), anticancer drugs, birth control pills,
vitamin A and its derivative, isotretinoin
which used in the treatment of severe acne.
Symptoms
- Increased shedding
of hair in excess of the normal loss of 50-100 hairs a day.
 |
Telogen effluvium.
Click
on image for larger view |
What you can do
- You should consult
a doctor.
- You can wear a wig
to conceal the hairloss until the hair grows back.
What the doctor
may do
- Confirm the diagnosis
by performing a telogen hair count (above 25%).
- Exclude underlying
diseases.
- Do nothing and wait
till the hair grows back.
- Prescribe minoxidil
lotion to promote hair growth.
TOP
TINEA
Tinea or ringworm is
a superficial fungal infection of the skin. The term "ringworm"
is actually inappropriate because there is no worm involved and
the ring-like expansion is due to the infection spreading. Different
terms are used according to the areas involved.
TOP
TINEA
AMIANTACEA
Tinea amiantacea causes
thick shiny asbestos-like scaling causing the hair to become
matted together. If crusting is thick, there may be a pussy exudate
under the crust and even alopecia (loss of hair). Tinae amiantacea
is believed to be related to psoriasis.
Treatment is the same as for psoriasis of the scalp.
 |
Tinae amiantacea.
Click
on image for larger view |
TOP
TRAUMATIC ALOPECIA
Traumatic alopecia
is a form of hairloss resulting from trauma.
Causes
- Traction alopecia - caused by tight braids and
pony tails.
- Hot-comb alopecia
due to attempts to straighten the hair.
- Pressure - seen in
the back of the heads of babies or people who lie on their backs
for prolonged periods.
- Trichotillomania - a self induced alopecia caused
by habitually plucking, pulling or cutting the hair. In children,
mild emotional problems may be present. In adults, there may
be underlying deep emotional and psychiatric problems.
- Burns - thermal, electrical
or chemical.
Symptoms
- The hairloss is patchy
and it's pattern depends on the type of trauma.
- Traction alopecia
usually occurs at the margins of the hairline, along the part
or scattered through the scalp depending on the hair style.
- Hot-comb alopecia
is usually seen in Blacks and affects the crown.
- Traumatic alopecia
due to burns occur at the site of injury.
- Trichotillomania causes
irregularly shaped angular areas of hairloss. The hairs within
the area are short or stubbly and broken off at different lengths.
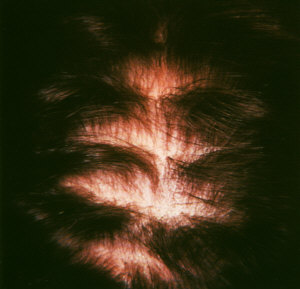 |
Traction alopecia.
Click
on image for larger view |
- What you can do
- Eliminate the cause,
if any, eg., change the hair style.
- You can consult a
doctor to confirm the diagnosis and cause.
What the doctor
may do
- Confirm the diagnosis.
- Excision of small
areas of traumatic alopecia caused by burns may be possible.
- Gently counsel children
with trichotillomania. Adult cases often have deep emotional
or psychiatric problems and may require referral to a psychiatrist.
TOP
TRICHOEPITHELIOMA
Trichoepithelioma is
an inherited condition that causes skin coloured or yellow bumps
around the centre of the face. It usually affects women.
Cause
- Inherited.
Symptoms
- Multiple small (less
than 1 cm) skin-coloured, slightly transcluscent rounded bumps
around the nose, on the cheeks and eyebrows.
 |
Trichoepithelioma.
Click
on image for larger view |
What you can
do
- You should consult
a doctor to confirm the diagnosis.
What the doctor
may do
- Perform a skin
biopsy to confirm the diagnosis.
- Treat for cosmetic
reasons. Excision, electrosurgery
and carbon dioxide laser
may be used.
TOP
TRICHOSTASIS SPINULOSA
Trichostasis spinulosa
is a harmless condition that affects the pores of some adults.
Cause
- Blockage of the hair
follicles which cause hairs to be retained in the follicle.
Symptoms
- Open pores which on
careful examination contain tiny short hairs. They are often
mistaken for blackheads.
- Usually occur on the
nose and sometimes, on the chest and back.
-
- What you can do
- You should consult
a doctor.
What the doctor
may do
- Reassure you.
- Treat with keratolytics
which help to unclog the pores.
TOP |





