|
V
Varicella | Varicose
eczema | Vasculitis | Vitiligo
VARICELLA
(CHICKENPOX)
Varicella or chickenpox
is a viral infection that causes fever and blisters which crust
over and heal after 2 to 3 weeks. It usually affects children
but can also occur in adults who may develop a more severe and
sometimes even fatal infection. The person becomes immune to
further attacks of varicella but may develop herpes
zoster (shingles) instead, later on in life.
Cause
- Varicella-zoster virus
(VZV) which is transmitted by airborne droplets and skin to skin
contact. The incubation period is 1 - 3 weeks. After infection,
the varicella-zoster virus travels up a nerve and remains dormant
(inactive) in the nerve ganglion (nerve relay station). If activated
(usually in late adult life), the virus causes a more localised
infection known as shingles (see herpes
zoster).
Symptoms
- Preceding malaise
(feeling of illness), headache, muscle ache and low-grade fever.
- Pink to red spots
which develop a blister in the centre giving rise to the appearance
of a "dewdrop on a rose petal".
- The vesicles become
pustules (pusheads) and crust over a 8 to 12 -hour period.
- The eruptions occur
in crops over the trunk, face and scalp so that at any one time
different evolutionary stages may be seen.
- Crusts will loosen
after another 1 - 2 weeks.
- Itching.
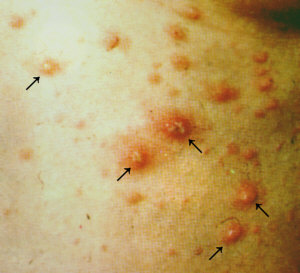 |
Varicella (chickenpox)
Click
on image for larger view |
Complications
- Scarring.
- Secondary bacterial
infection which increases the risk of scars.
- Secondary bacterial
infection may get into the blood and cause septicaemia (blood
poisoning).
- Pneumonia (lung inflammation).
- Encephalitis (brain
inflammation).
- Death which is more
common in adults.
- Congenital varicella
may develop if infection occurs in the first 3 months of pregnancy,
resulting in an underweight baby with eye and brain abnormalities,
scarring of the skin and abnormal development of the limbs.
What you can do
- You should consult
a doctor.
- Take antihistamines
to relieve itching.
- Avoid scratching as
it encourages secondary infection and scarring.
- Apply cool compresses.
- Apply calamine lotion
to reduce itching.
- Stay in isolation.
Varicella is infectious 5 days before the onset of the rash until
all the eruptions have crusted.
- Take paracetemol for
fever relief. Do not take aspirin as this has been associated
with the development of Reye's syndrome, a life-threatening condition
causing brain and liver inflammation.
What the doctor
may do
- Confirm the diagnosis.
- Prescribe topical
or oral antibiotics.
- Prescribe oral acyclovir
which helps to reduce the severity of symptoms and hasten healing.
Prevention
- A vaccine is now available
to prevent varicella.
TOP
VARICOSE
ECZEMA
Varicose eczema or
stasis dermatitis is a form of eczema affecting the legs of people
with varicose veins. Women are more likely to be affected because
they have a higher risk of developing varicose veins.
Cause
- Poor return of blood
from the leg veins to the heart, results in the pooling of blood
in the veins, causing varicose veins as well as a diminished
supply of oxygen to the tissues there. The latter is believed
to cause varicose eczema.
Symptoms
- Redness and scaling,
occasionally with weeping and crusting on the lower portion of
the legs, especially on the inside of the ankles.
- Brownish pigmentation
of the skin.
- Fibrosis or stiffening
of the skin.
- Varicose veins or
thin threadlike blue veins around the ankles are usually (but
not always) evident.
 |
Varicose (stasis) ulcer.
Click
on image for larger view |
Complications
- Ulceration.
- Secondary bacterial
infection.
- Allergies often develop
to topical medications used on the area.
What you can do
- You should consult
a doctor.
- Avoid scratching as
this may cause ulceration and secondary bacterial infection.
- Apply saline compress
if the area is weepy.
- Take antihistamines
to reduce itch.
- Wear compression bandages
or supportive stockings.
- Raise the foot of
the bed by about 10 inches to help return blood.
- Lose weight if obese.
- Exercise or stretch
the legs regularly.
- Put up the feet as
often as possible.
- Avoid constricting
garments.
- Avoid constipation
by taking high fibre diet.
What the doctor
may do
- Prescribe topical
steroids.
- Prescribe antibiotics
for secondary bacterial infection.
- Conduct patch
tests to determine the cause of allergy, if necessary.
- Sclerotherapy (injections
to force closure of the varicose veins) or surgery to remove
the varicose veins.
- Pinch grafts to help
ulcers heal.
TOP
VASCULITIS
Vasculitis is an inflammation
of the blood vessel walls due to an immunological reaction. It
can be divided into cutaneous vasculitis which affects the blood
vessels of the skin and systemic vasculitis which affects the
blood vessels supplying internal organs such as heart, kidneys,
intestines, muscles and nervous system. There are many forms
of vasculitis, some involving only the blood vessels in the skin
primarily and are painful but otherwise harmless. Others like
polyateritis nodosa and Wegener's granulomatosis involve blood
vessels supplying the heart, kidneys, intestines, muscles and
nervous system are potentially serious.
Causes
- Drugs and injected
serum.
- Infections such as
streptococcal sorethroat (Henoch Schonlein purpura) and hepatitis
B (polyarteritis nodosa).
- Collagen vascular
disease such as lupus erythematosus
and rheumatoid arthritis.
- Lymphoma (cancer of
the lymph glands).
- Blood disorders.
- Idiopathic (of unknown
cause).
Symptoms
- Purpura (haemorrhagic
spots or patches) which is slightly raised. Purpura does not
disappear when pessed.
- Blisters, painful
nodules (swellings) and ulcers may occur in more severe cases.
- Urticarial vasculitis which is different from ordinary
urticaria in that it lasts more
than 24 hours and heals with a dark stain.
- Livedo reticularis which is a mottled or net-like
bluish or purplish discolouration of the skin. It may be a sign
of polyarteritis nodosa which may affect the skin alone (cutaneous
polyarteritis nodosa) or the skin and internal organs (systemic
polyarteritis nodosa).
- Henoch-Schonlein
purpura (HSP)
is a type of vasculitis that is associated with joint pains,
abdominal pains (sometimes constipation or diarrhoea) and haematuria
(blood in the urine). It represents a hypersensitivity reaction
caused by streptococcal throat infections.
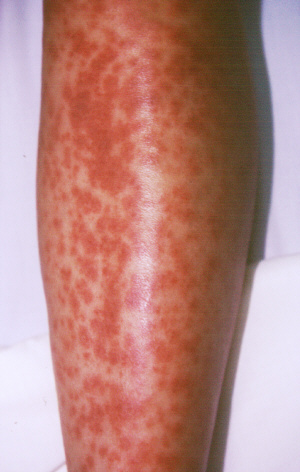 |
Vasculitis.
Click
on image for larger view |
- Complications
Complications are usually caused by vasculitis affecting internal
organs, for example,
- Systemic polyarteritis
nodosa may cause fever, joint and muscle pains, nausea, vomiting,
abdominal pain, heart failure, high blood pressure, kidney problems,
strokes and nerve damage.
- Wegener's granulomatosis
may also affect the larger blood vessels, mouth, ear nose and
throat (ulcers and destruction of the nasal cartilage leading
to a saddle nose deformity), lungs (coughing of blood and breathlessness),
eye, kidney and nerve inflammation.
What you can do
- You should consult
a doctor.
What the doctor
may do
- Perform a skin
biopsy.
- Conduct tests to exclude
involvement of internal organs.
- Treat with systemic
steroids, anti-inflammatory
and immunosuppressive
drugs.
- Treat the underlying
cause, if any.
TOP
VITILIGO
Vitiligo or leucoderma
occurs when the skin pigment, melanin is not produced. It affects
about 1% of the population and is a serious cosmetic problem
in dark-skinned individuals. A familial tendency has been observed.
Cause
- Autoimmune disease
(self-allergy) in which the body's defence system mistakenly
attacks the melanocytes (melanin-producing cells) as though they
were foreign.
Symptoms
- Well-defined milky
white patches.
- Occurs most commonly
on the face, neck, hands, elbows, knees, the body folds such
as the armpits and groin, nipples, genital areas, around orifices
(mouth, eyes, anus, umbilicus) and on areas of trauma (eg., along
scratch lines).
- May have evidence
or a history of other autoimmune diseases such as premature greying
of the hair (see canities), alopecia areata, diabetes,
pernicious anaemia, Addison's disease and thyroid disease.
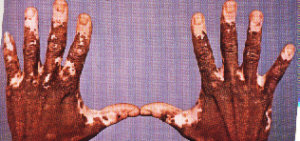 |
Vitiligo.
Click
on image for larger view |
- Complications
- Very occasionally,
vitiligo may spread to involve very extensive areas of skin.
What you can do
- You should consult
a doctor.
- Use cosmetic camouflage.
What the doctor
may do
- Exclude other autoimmune
diseases or check for antibodies to thyroglobulin and parietal
cells (which are increased in autoimmune disorders).
- Prescribe topical
steroids.
- Treat with topical
or oral PUVA - natural or
artificial sunlight in association with psoralens (a photosensitising
medicine that may be applied to the skin or taken by mouth).
- Minigrafting which
involves removing circular areas of depigmented skin with a biopsy
punch and replacing them with grafts taken with the same instrument
from other sites such as the buttocks.
- Bleach the remaining
skin to a uniform white colour if vitiligo is very extensive.
- Keypoints
- The treatment of vitiligo
is not very satisfactory.
- Repigmentation is
slow and may not be complete, especially over the fingers and
bony prominences.
- Repigmentation is
unlikely if the area involved has no hair follicles or the hairs
there are white.
TOP |


