|
M
Male pattern baldness
(go to androgenetic alopecia)
| Mastocytosis | Measles
| Melanomas | Melasma
| Milaria | Moles
| Morphoea (see scleroderma)
| Molluscum contagiosum
| Mongolian spot | Moniliasis (go
to candidiasis) | Mucous
cyst | Mycosis fungoides
MASTOCYTOSIS
Mastocytosis refers
to abnormal collections of mast cells in the skin. Mast cells
are large cells with granules containing chemicals such as heparin,
serotonin and histamine. When mast cells degranulate, these chemicals
(notably histamine) are released, causing urticaria (weals),
redness and itching.
- Mastocytosis is classified
into the following varieties:
- Cutaneous mastocytosis
when only the skin is affected
-
- Mastocytoma (usually
solitary).
- Urticaria pigmentosa
(usually multiple).
- Diffuse cutaneous
mastocytosis.
- Telangiectasia eruptiva
macularis perstans.
-
- Systemic mastocytosis
when internal organs are involved.
Cause
- Unknown.
Symptoms
- Single or multiple
brown or orange brown papules (bumps) or patches that itch, swell
and sometimes blister when stroked.
- May occur on the body,
neck or arm, especially near the wrist.
- Usually affects children
at birth or within the first 1 year. It may occasionally affect
adults, as well.
- In some patients,
the urticaria pigmentosa is more freckle-like and causes the
skin to develop a darkened appearance with small telangiectasias
(broken capillaries) on the surface. This form is known as telangiectasia
eruptiva macularis perstans.
- Diffuse cutaneous
mastocytosis may cause a yellowish thickening of the skin or
erythroderma.
- The diagnostic sign
of cutaneous mastocytosis is known as Darier's sign wherein the
affected area swells, developes a weal or blisters when it is
rubbed.
- Systemic mastocytosis
may cause enlargement of the liver, spleen and lymph glands or
affect the bones and the gastrointestinal tract.
- Childhood cases of
cutaneous mastocytosis usually resolve on their own, usually
by adolescence. Adult cases tend to be more persistent.
Complications
- Extensive urticaria
pigmentosa may cause symptoms of histamine release such as flushing,
nausea, vomiting, upper stomach pain and even shock. This usually
occurs when the person takes drugs that cause the mast cells
to degranulate.
- Adults with urticaria
pigmentosa or telangiectasia macularis eruptiva perstans may
sometimes go on to develop systemic mastocytosis.
- Some patients with
systemic mastocytosis may go on to develop mast cell leukaemia
where malignant mast cells can be found circulating in the blood.
What you can do
- You should consult
the doctor.
- Avoid drugs that cause
mast cells to degranulate. Examples include alcohol and codeine.
Other drugs to watch out for include dextran, polymyxin B, morphine,
scopolamine and d-tubocurarine which may be used by doctors.
What the doctor
may do
- Perform a skin biopsy
to confirm the diagnosis.
- Examine and investigate
for other organ involvement.
- Prescribe oral antihistamines,
topical steroids
or oral disodium cromoglycate (which is a mast cell stabiliser).
PUVA and interferon may be
used in adults with severe urticaria pigmentosa.
- Follow-up closely.
TOP
MEASLES
Measles is a childhood
viral infection that affects the skin, eyes and the respiratory
system.
Cause
- Measles virus which
is transmitted through droplet infection. The incubation period
is 10 - 14 days.
Symptoms
- Measles usually begins
with high fever and cold symptoms such as runny nose, conjunctivitis
(red eyes) and a dry hacking cough.
- The rash appears 3
- 4 days later, along the hairline and around the ears and then
spreads downwards to the face, trunk and limbs. The rash begins
as numerous red spots which later join to form large red blotches.
After about 3 days, the rash fades in the order it appears with
bran-like shedding of skin scales.
- Koplik's spots (white spots) on the inside
of the cheeks opposite the premolar teeth are diagnostic of measles.
These spots appear on the second or third day of the fever and
disappear a few days after the rash appears.
- There may be a generalised
enlargement of the lymph glands. Photophobia or intolerance of
bright lights is common.
Complications
- Otitis media (inflammation
of the middle ear).
- Pneumonia (lung inflammation).
- Encephalitis (brain
inflammation), causing headache, nausea, vomiting, epilepsy and
coma.
- Sclerosing panencephalitis,
a rare progressive brain disorder may develop many years after
the infection.
- Death may very rarely
result from complications such as pneumonia and encephalitis.
- There is a 25% risk
of feotal death when measles occurs in a pregnant women.
What you can do
- You should consult
a doctor for confirmation and to exclude complications.
- Rest, drink lots of
fluid.
- Take fever medicines
(not aspirin as its use has been associated with the development
of Reye's syndrome, a life-threatening condition causing brain
and liver inflammation.
- Take antihistamines
and apply a soothing lotion such as calamine to relieve itching.
- If a child has fever
above 38.5oC, sponge to bring the temperature down and reduce
the risk of febrile fits.
- Use dim lighting if
the eyes are irritated by bright lights.
- Go to the hospital
immediately if vomiting, epilepsy or breathing difficulties develop.
Prevention
- Measles can be prevented
by vaccination. Most children are vaccinated at 1 - 3 years of
age.
What the doctor
may do
- Confirm the diagnosis.
- Treat the complications.
TOP
MELANOMAS,
MALIGNANT MELANOMAS
Malignant melanomas
or cancerous moles are the most feared skin cancers because of
their potential to spread to other parts of the body. They are
more common among fair-skinned individuals, especially those
of Northern European or Celtic origin and may arise in pre-existing
moles such as congenital and dysplastic naevi.
Causes
- A cancer arising from
the melanocytes or pigment cells.
-
- Predisposing factors
- Fair skin types I
and II with a history of over-exposure to the sun.
- A history of severe
sunburns during childhood increases the risk of melanoma developing.
- Inherited tendency.
The risk of melanoma is increased if there is a family history
of melanoma.
- Dysplastic naevi (atypical
moles). Non-familial or sporadic cases are associated with a
slightly increased risk of developing malignant melanoma but
familial dysplastic naevi with a family history of melanoma in
two or more close relatives is associated with an almost 100%
lifetime risk of developing a melanoma.
- Large or giant congenital naevi are associated
with a higher risk of developing malignant melanoma.
Symptoms
Malignant melanomas may arise on normal skin or in a pre-existing
naevus such as congenital naevi and dysplastic naevi.
- Melanomas are usually
uneven in colour and and have a irregular outline. They may have
any combination of brown, black, blue grey or black. Amelanotic
melanomas are skin-coloured rather than pigmented.
- Untreated, melanomas
grow in size and thickness and become nodular. They may eventually
ulcerate and bleed.
- A particular type
of melanoma known as acral lentiginous melanoma occurs
on the extremities such as the palms, soles, fingers and toes.
It is the most common type of melanoma in Asians and blacks.
Sometimes, it may occur as a black streak in the nail.
- Lentigo maligna is a type of early melanoma
that occurs on the sun-exposed skin of the elderly.
The
American Academy of Dermatology's ABCD signs lists
the danger signs to look out for in a mole. These signs are essentially,
also those of a dysplastic naevus-
-
- Asymmetry which means one side
does not match the other.
- Borders that are irregular.
- Colour variation within the
lesion such as various shades of red and blue mixed with areas
of black, white or brown.
- Diameter over 6mm.
Other signs to
watch out for include:
-
- A mole that appears
for the first time after the age of 35 years.
- Bleeding, oozing,
crusting or ulceration.
- Pain, tenderness or
itching.
- Inflammation around
the mole.
- Nodule developing
in the centre.
 |
Malignant melanoma.
Click
on image for larger view |
Complications
- May spread to internal
organs, causing death.
What you can do
- You should consult
a doctor if you have a suspicious mole because early removal
or melanomas can result in cure.
- You should examine
your skin regularly, especially if you have the predisposing
factors mentioned above. It is a good idea to get your spouse
or a close relative to check your back regularly, as well.
- Melanomas can be prevented
by protecting the skin against the sun (see sun
protection).
- Drink alcohol in moderation
because there is evidence to suggest that alcohol may increase
the risk of developing melanomas.
What the doctor
may do
- Perform a skin
biopsy to confirm the diagnosis and stage the melanoma. The
pathologist reading the microscopic slide also measures the thickness
of the melanoma and the level of penetration (known as Clark's
level). Thin melanomas that are less than 0.76mm thick are unlikely
to cause fatalities.
- The doctor may need
to remove a wider area of skin around the melanoma.
- In more advanced cases,
the lymph glands draining the area may also need to be removed.
- Chemotherapy or immunotherapy
may be used in very advanced cases.
- Long-term follow-up
is necessary.
TOP
MELASMA
Melasma or chloasma
is a blotchy type of facial pigmentation, most commonly seen
in women.
Causes
- Unknown.
- Pregnancy (hence,
its other name "mask of pregnancy") and the birth control
pill may precipitate it.
- Sun-exposure makes
melasma worse.
- Racial factors may
be important as melasma is more common among darker-skinned persons.
- Inheritence may also
play a role as melasma tends to run in families.
Symptoms
- Yellow brown to black
blotches on the face, especially the cheeks, forehead, nose and
upper lip.
- The blotches usually
darken on exposure to the sun.
 |
Melasma.
Click
on image for larger view |
Key point
- Melasma may sometimes
be due to a phototoxic contact dermatitis to perfumes found in
after-shave lotions (especially musk-ambrette)
and scented toiletries.
What you can do
- Nothing since it is
a cosmetic problem.
- Use cosmetics to camouflage
the pigmentation.
- Protect the skin against
the sun (see sun protection).
What the doctor
may do
- Prescribe lightening
creams containing hydroquinone alone or a combination
of hydroquinone and tretinoin with or without a steroid.
- Perform superficial
or medium depth chemical peels.
- Remove the aggravating
cause eg., discontinue the birth control pill.
- Counsel you on sun protection.
TOP
MILARIA
Milaria (prickly heat
or heat rash) is common in children, adolescents and young adults
living or working in hot humid environments. It is more common
during the first few weeks of life because the sweat ducts have
not fully developed and get blocked easily.
Cause
- Milaria occurs when
sweat cannot evaporate but is absorbed into the skin causing
it to swell and block the opening of the sweat duct.
Symptoms
- The mild form, milaria
crystallina appears as tiny, clear blisters.
- The more severe form
appears as pin-head size blisters or pusheads surrounded by redness
on the chest and back where there is a higher concentration of
sweat glands and on areas of the skin where the surfaces touch
each other such as the neck, under the arms, in the groins, in
the skin folds of plump babies and obese adults. The inflamed
variety is called milaria rubra (red papules) or milaria
pustulosa (when there are pusheads).
- Itching and a prickly
burning sensation may occur in milaria rubra and milaria pustulosa.
 |
Milaria rubrum.
Click
on image for larger view |
Complications
- Milaria interferes
with sweating and the ability of the body to cool itself. Heat
stroke may develop if milaria is extensive.
- Secondary infection
by bacteria or fungi..
What you can do
- The aim is to reduce
excessive sweating and humidity:
- Wear light cotton
clothing and loose clothing.
- Avoid high temperatures
and humidity. Use fans or air conditioning.
- Limit physical activity
if possible.
- Take cool baths or
showers regularly.
- Dry well.
- Calamine lotion may
be helpful.
- Taking vitamin C,
1g daily may be helpful.
- Consult a doctor if
there is no improvement after a week.
What the doctor
may do
- Confirm the diagnosis.
- Prescribe mild topical
steroids.
- Treat the complications.
TOP
MOLES
OR MELANOCYTIC NAEVI
Melanocytic naevi (naevi
is plural for naevus) or common moles are usually not present
at birth but appear in later life, especially during puberty
and pregnancy. Most adults have on average about 20 moles. Moles
that appear at birth are called congenital moles.
Cause
- Non-cancerous proliferation
of melanocytes (pigment cells).
- Symptoms
Melanocytic naevi may be flat or raised, hairy or hairless and
their colours vary from skin coloured to pink, brown or black.
However, they all show symmetry, regular outlines and are evenly
coloured. Any departure from this should be viewed with suspicion
(see ABCD signs). The different types
of moles include:
- Junctional naevi
- These are flat and
dark brown or black.
-
- Intradermal naevi.
- These are elevated,
skin coloured, brown or black and may be smooth or warty.
-
- Compound naevi.
- These are usually
elevated, dome-shaped, skin-coloured, brown or black. and may
have hairs growing out of them.
-
- Halo naevi (Sutton's
naevi, leukoderma acquisitum centrifugum)
- These are moles that
have a pale halo around them. They usually occur in children
and young adults.
-
- Blue naevus
- These are deep moles
which are blue because the pigment lies deeper in the skin. They
usually occur in children and young adults.
-
- Congenital
naevi.
- These are moles that
appear at birth. They may be hairy and may quite large, sometimes
covering a large segment of the skin or an entire limbs.
-
- Dysplastic
naevi (atypical
moles)
- These are moles that
show atypical features (see American Academy of Dermatology's
ABCD signs).
 |
Compound mole.
Click
on image for larger view |
Complications
- Most moles do not
become cancerous. However, there is a higher cancer risk in large
congenital naevi and in dysplastic naevi and this is why people
with these moles need to be closely followed up by a dermatologist
(skin specialist). Look out for the following:
-
- Asymmetry which means one side
does not match the other.
- Borders that are irregular.
- Colour variation within the
lesion such as various shades of red and blue mixed with areas
of black, white or brown.
- Diameter over 6mm.
- Change in a pre-existing
mole such as:
-
- Bleeding, oozing,
crusting or ulceration.
- Pain, tenderness or
itching.
- Inflammation around
the mole.
- Nodule developing
in the centre.
What you can do
- You should consult
a doctor if any of the above changes occur.
- See a doctor if you
want a mole removed for any reason.
- Do not irritate the
mole or pluck hairs from a mole. Cut the hairs off carefully
if you want to.
-
- What the doctor
may do
- Confirm the diagnosis.
- Remove suspicious
looking moles.
- Excise for cosmetic
reasons.
TOP
MOLLUSCUM CONTAGIOSUM
Molluscum contagiosum
(water wart) is a viral infection of the skin that affects children,
especially those with atopic
dermatitis and young adults. Infection is transmitted by
skin-to-skin contact including sexual intercourse (adults cases).
Cause
- Pox virus. Infection
is transmitted by skin to skin contact in children or during
sexual contact in adults.
Symptoms
- Pearly-white or skin
coloured papules (pimply bumps), often with central pit or depression.
- Size between 2 - 5
mm.
- Tendency to occur
in groups or in lines along scratch marks.
- Occurs on the genitals
of adults (where it is usually sexually transmitted) or anywhere
on the face and body of children.
 |
Molluscum contagiosum.
Click
on image for larger view |
What you can
do
- You should consult
a doctor. Although, molluscum contagiosum can clear on their
own, this may take several months to 2 years and there is a risk
of transmitting infection to other people.
- Do not pick or scratch
as this causes the infection to spread to other areas.
How the doctor can
help
- Treat using electrosurgery,
liquid nitrogen, curettage, application of
trichloroacetic acid or cantharidin, tretinoin
(Vitamin A acid) cream and salicylic acid.
TOP
MONGOLIAN
SPOT
This is a type of pigmented
birthmark that occurs at birth. It is seen more commonly in Asian
and black babies.
Cause
- Benign proliferation
of melanocytes (pigment cells) within the dermis.
Symptoms
- Blue-black patch on
the buttocks or near the base of the spine (may be misdiagnosed
as child abuse).
What you can do
- Nothing as they will
disappear on their own.
- See a doctor to confirm
the diagnosis.
What the doctor
may do
- Confirm the diagnosis.
- Reassure you that
it will disappear with time.
TOP
MUCOUS
CYST
This is a type of cyst
that usually occurs in the lower lip of young and middle-aged
adults.
Cause
- Blockage or rupture
of the salivary gland.
-
- Symptoms
- Bluish coloured cyst,
usually on the inner surface of the lower lip.
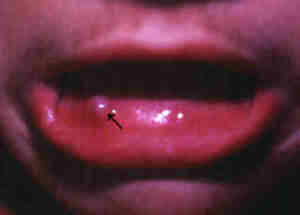 |
Mucous cyst.
Click
on image for larger view |
What you can do
- ou should consult
a doctor.
- Do not pierce or bite
the cyst.
What the doctor
may do
- Remove using electrosurgery,
carbon dioxide laser
or by surgical excision. Recurrences are quite common.
- Incision and draining
the jelly-like fluid inside the cyst. This is usually temporary
as the cyst often recurs.
TOP
MYCOSIS FUNGOIDES
This is a type of lymphoma
(lymphatic cancer) that affects the skin. It is also called cutaneous
T-cell lymphoma CTCL.
Cause
- A type of cancer arising
from the T-lymphocytes (a special type of white blood cell).
Symptoms
- Persistent red scaly
patch which may be mistaken for eczema
or psoriasis.
- Over time, the patch
becomes thicker and developes into a plaque or becomes nodular
and may even ulcerate.
- Mycosis fungoides
may affect any part of the body but is more common on the back,
buttocks and shoulders.
- There may or may not
be itching.
- Usually affects middle-aged
and elderly individuals.
- May involve the whole
body as an erythroderma. This type of mycosis fungoides is called
Sezary syndrome and may be associated with abnormal white
cells known as Sezary cells in the blood. Sezary syndrome is
considered to be the leukaemic stage of mycosis fungoides..
 |
Mycosis fungoides.
Click
on image for larger view |
Complications
- May spread internally
to other organs.
- May be fatal.
What you can do
- You should consult
a doctor.
What the doctor
may do
- Perform a skin
biopsy to confirm the diagnosis.
- Perform tests to exclude
other organ involvement
- Treat with UV-B
or PUVA, anti-cancer drugs,
nitrogen mustard.
TOP |





