|
N
Naevus
of OTA | Naevus sebaceum | Napkin
dermatitis | Nappy rash (go to napkin
dermatitis) | Necrobiosis lipoidica
| Neurofibroma | Neuorodermatitis
(go to lichen simplex chronicus)
| Nummular dermatitis or discoid
eczema
NAEVUS
OF OTA
This is a type of pigmented
birthmark that is more common in Orientals and Blacks. It may
occur at birth or during the first two decades of life and persists
indefinitely. Women are more commonly affected.
Cause
- Non-cancerous proliferation
of melanocytes (pigment cells) in the dermis (deeper layer of
the skin).
Symptoms
- Blue-black or grey
pigmentation around one eye.
- The sclera (white
of the eye) may be afected, as well
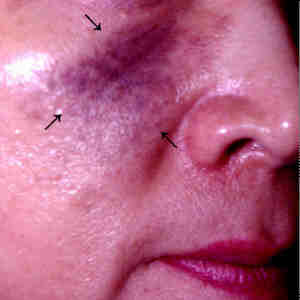 |
Naevus of Ota.
Click
on image for larger view |
What you can
do
- Nothing, live with
it.
- Use cosmetic camouflage.
- Consult a doctor for
treatment
What the doctor
may do
- Treat with one of
the pigment lasers.
Top
NAEVUS
SEBACEUM
This is a developmental
abnormality affecting the scalp.
Cause
- Developmental abnormality
arising from the sebaceous glands.
Symptoms
- Appears at or shortly
after birth
- Yellowish orange elevated
patch on the scalp associated with some degree of hairloss.
Complications
- May develop into basal
cell or some other cancers.
What you can do
- You should consult
a doctor for removal because of the cancer risk.
What the doctor
may do
- Excise the naevus
or destroy with electrosurgery
or the carbon
dioxide laser.
Top
NAPKIN DERMATITIS
Napkin dermatitis,
diaper dermatitis or nappy rash is a common skin problem in infants
and young children who are not yet potty trained.
Causes
- Prolonged contact
of the skin with urine and faeces in soiled nappies is the main
cause.
- Irritation caused
by antiseptics and disinfectants used for cleaning nappies.
- Skin conditions such
as seborrhoeic dermatitis,
atopic dermatitis and
psoriasis affecting the napkin
area.
Symptoms
- Redness and swelling
or blistering and ulceration in severe cases.
- In chronic cases,
the area becomes red and scaly.
- Affects the napkin
area but typically spares the apex of the groin crease which
does not come into direct contact with soiled nappies.
Complications
- The moist environment
encourages the development of secondary candidiasis
(yeast infection).
- What you can do
- Prevention is better
than cure and the most important strategy is to keep the area
clean and dry.
- Apply wet compresses
to reduce inflammation.
- Cleanse with water
after each passage of urine or stool, pat dry and apply a water
repellent formula such as white soft paraffin, silicone cream
or zinc oxide ointment.
- Expose to air as often
as possible.
- Change nappies as
soon as they are soiled.
- Wash nappies thoroughly
to remove antiseptics and detergents. It helps to add an ounce
of household vinegar to a gallon to water during the final rinse
to adjust the pH closer to the skin pH.
- Consult a doctor if
it there is no improvement. It may indicate candidiasis
or underlying skin disease such as seborrhoeic
dermatitis, atopic dermatitis
or psoriasis.
What the doctor
may do
- Prescribe a mild topical
steroids.
- Take skin scrapings
to exclude candidiasis.
- Prescribe topical
antifungals if candidiasis
is present.
Top
NECROBIOSIS
LIPOIDICA
This is a degenerative
skin condition that is often, though not always, associated with
diabetes.
- Cause
- Inflammation and degeneration
of collagen tissues in the skin, possibly as a result of diabetes
affecting the small blood vessels in the skin..
Symptoms
- Begins as one or more
dusky red plaques (raised patches) on the shins.
- These enlarge in size
and the centre becomes slightly depressed, thinned and waxy yellow
in colour. Telangiectasias
(broken capillaries) can usually be seen through the thinned
skin.
 |
Necrobiosis lipoidica.
Click
on image for larger view |
Complication
- The skin is fragile
and can be easily traumatised, leading to ulcers.
What you can do
- You should consult
a doctor.
- Protect the area from
injury.
- Make sure that your
diabetes is well controlled.
What the doctor
may do
- Perform a skin
biopsy to confirm the diagnosis, if necessary.
- Perform blood and
urine tests to exclude diabetes unless already diagnosed.
- Control diabetes with
drugs and dietary advice.
- Treat with topical
steroids or intralesional steroids.
- Prescribe oral pentoxifylline
which helps to improve blood circulation.
Top
NEUROFIBROMA
Neurofibromas are soft
skin growths arising from the nerve sheath. They may be solitary
or multiple. The term neurofibromatosis or von Recklinghausen's
disease is used when neurofibromas are multiple and associated
with other abnormalities (see below). Neurofibromatosis or von
Recklinghausen's disease is inherited and usually occurs during
adolescence whereas solitary neurofibromas usually occur in adults.
Causes
- Non-cancerous or benign
growth of the nerve sheath. Neurofibromatosis or von Recklinhausen's
disease is inherited in an autosomal dominant fashion which means
that only one parent need to be affected and the offsprings have
a 50% chance of inheriting and developing the disorder.
Symptoms
- Single or multiple,
soft, skin-coloured nodules (swellings).
- The nodule can be
pressed into the skin with the finger tip. Doctors call this
the button-hole sign and this is diagnostic of neurofibromas.
- The nodules increase
in size over time and may become pedunculated.
- Occasionally, the
nodules may form large folded or pendulous masses known as plexifom
neurofibromas. Sometimes a whole limb is affected, causing
elephantiasis.
- Multiple cafe-au-lait
patches (which means "coffee with milk" patches),
freckles in the armpits and groins and kyphoscoliosis (curvature
of the spine) are other signs associated with von Recklinghausen's
disease.
- Neurofibromas may
sometimes affect the central nervous system, optic nerves of
the eyes, the eight nerve (which) and spinal column.
Complications
- Severe cosmetic disfigurement,
especially if there are hundreds or thousands of neurofibromas.
- Cancerous change may
occasionally occur in plexiform neurofibromas.
- Bone and spine curvatures
(eg., kyphoscoliosis).
What you can do
- You should consult
a doctor.
What the doctor
may do
- Perform a skin
biopsy to confirm the diagnosis.
- Refer you to a ophthalmologist
for a slit-light examination of the eyes
- Excise disfiguring
swellings or those that have increased rapidly in size or are
painful.
- Provide genetic counseling
for patients with von Recklinghausen's disease.
- Follow up cases of
plexiform neurofibromas so that any cancerous change can be detected
early.
Top
NUMMULAR DERMATITIS OR DISCOID ECZEMA
Nummular (nummulus
in Latin means coin-shaped) dermatitis or discoid eczema causes
coin-shaped patches of eczema. It occurs more commonly outside
the 30 - 50 year age group.
Causes
- Usually regarded as
a type of endogenous or constitutional eczema.
May be a variety of atopic dermatitis in children.
- May be caused by allergy
to nickel (found in metals) and chromates (in cement).
Aggravating factors
- Xerosis or dry skin.
- Dry winters.
- Irritation from rough
fabrics.
- Stress.
Symptoms
- Starts as small blisters
or papules (bumps) which rapidly join to form plaques (elevated
patches).
- The plaques are typically
round or coin-shaped and often become weepy and crusted.
- They usually affect
the front of the legs, back of the forearms and buttocks and
occasionally, the trunk, as well.
- The surrounding skin
is may be dry or xerotic (see xerosis).
- Itching is often severe.
 |
Nummular dermatitis or
discoid eczema.
Click
on image for larger view |
Complications
- Secondary bacterial
infection.
- Tendency to recur.
What you can do
- You should consult
a doctor.
- Take antihistamines
to relieve itching.
- Avoid scratching.
- Keep the skin well
moisturised because dry skin increases the likelihood of relapse.
- Avoid woolen and rough
textured fabrics.
What the doctor
may do
- Prescribe topical
or in severe cases, even systemic steroids.
Intralesional
steroids may be used to treat very resistant patches.
- Prescribe antibiotics
for secondary bacterial infection.
- Phototherapy (UV-B or PUVA) may be used
to treat severe and widespread cases.
Top |


